Introduction
Hemodialysis patients experience high levels of pain, fatigue, insomnia, and depression. The treatment regimen and frequency of treatment affect them, leading them to both dysfunction—as they are often unable to perform basic daily activities—and psychological burden, giving rise to conditions such as depression, intense anxiety, social alienation, and reduced well-being.1 Social support for patients with chronic kidney disease (CKD) is a key pillar of quality of life, as it is inextricably linked to well-being, acceptance of the new situation, and increased life expectancy. Patients starting hemodialysis are vulnerable and have an increased need to feel support and understanding from their social and family environment.2
In patients undergoing hemodialysis (HD) and receiving social support, it has been observed that they have higher levels of health – related quality of life (HRQoL) and better manage the emotional and physical needs of AMC3; it reduces the phenomena of social isolation and strengthens psychological resilience.4 It is also important to mention that it reduces levels of depression and actively contributes to increasing the quality of life.5 In addition, social support seems to have a significant impact on reducing anxiety. It has been shown that individuals who are shielded with social support activate active mechanisms to deal with situations that cause them intense stress.5 Emotional and physical support are the main categories that we identify in these patients, and this is due to the fact that these patients rely on their family and friends to carry out their obligations and for their emotional support.6 In recent decades, the need for social support has increased dramatically. Social support, combined with psychoeducational programs that are carried out with the aim of strengthening and supporting the social environment and caregivers of patients with CKD undergoing AMC, leads to high levels of mental well-being and physical health.7 A critical role in promoting social support is played by health professionals, who must create an environment that supports patients and connects them with a support network. This need has become more urgent than ever due to the rapid proliferation of patients enrolled in the HD.8
Spirituality can often influence the progression of the disease and the choice of treatment regimen, HRQoL, as well as the patient’s interpersonal relationships with loved ones. More specifically, in patients with chronic diseases such as CKD, the spiritual beliefs of patients contribute significantly to increasing HRQoL and psychosocial adjustment to their disease.9 A reasonable percentage of patients with end-stage CKD are dependent on spirituality and religion in order to cope with the disease that affects their quality of life. Spirituality functions as a support for chronic patients by giving meaning to life, death, and the disease itself.10
Family support and well-being significantly enhance adherence to treatment regimens and self-management in patients with CKD. Patients who enjoy social support from their family members adhere to their treatment regimen to a greater extent, as family members ensure that medical instructions are followed, monitor, remind, and help the patient take their medication, and prepare appropriate meals with the indicated restrictions.11 They also support patients by advising them to avoid prohibited foods and excessive fluid intake, making it easier for them to comply with the treatment plan. Patients living within a family also benefit from the observation of contraindications to medication by their family members, as the patient himself may not perceive changes that may occur in his body or may consider them a normal development and therefore not convey the information to health professionals.
In a study conducted in 2021 by Bôas & Nakasu, who investigated the effect of spirituality on medication adherence in patients undergoing hemodialysis, they demonstrated that there was a positive correlation between medication adherence and the development of the individual’s spirituality. This was evident from the higher scores obtained by patients who had attended spiritual practices compared to other patients.12
In spite of the fact that many studies have been conducted regarding quality of life in the group of hemodialysis patients, relevant studies are limited concerning all the variables that are examined in the present study, not only in the Greek literature but also in the foreign literature. Moreover, the research findings are often controversial.
The purpose of this research was to investigate quality of life and medication adherence among patients undergoing hemodialysis, as well as the association with clinical parameters, perceived social support, and spiritual needs.
Materials and methods
This is a cross-sectional observational study aimed at finding the effect of factors such as spirituality and social environment on the quality of life and level of medication adherence in patients suffering from CKD. This study was reported in accordance with the STROBE guidelines. The choice of this type of study was due to the particularly useful and valid results that arise from it when investigating the relationship between determinants and outcomes.
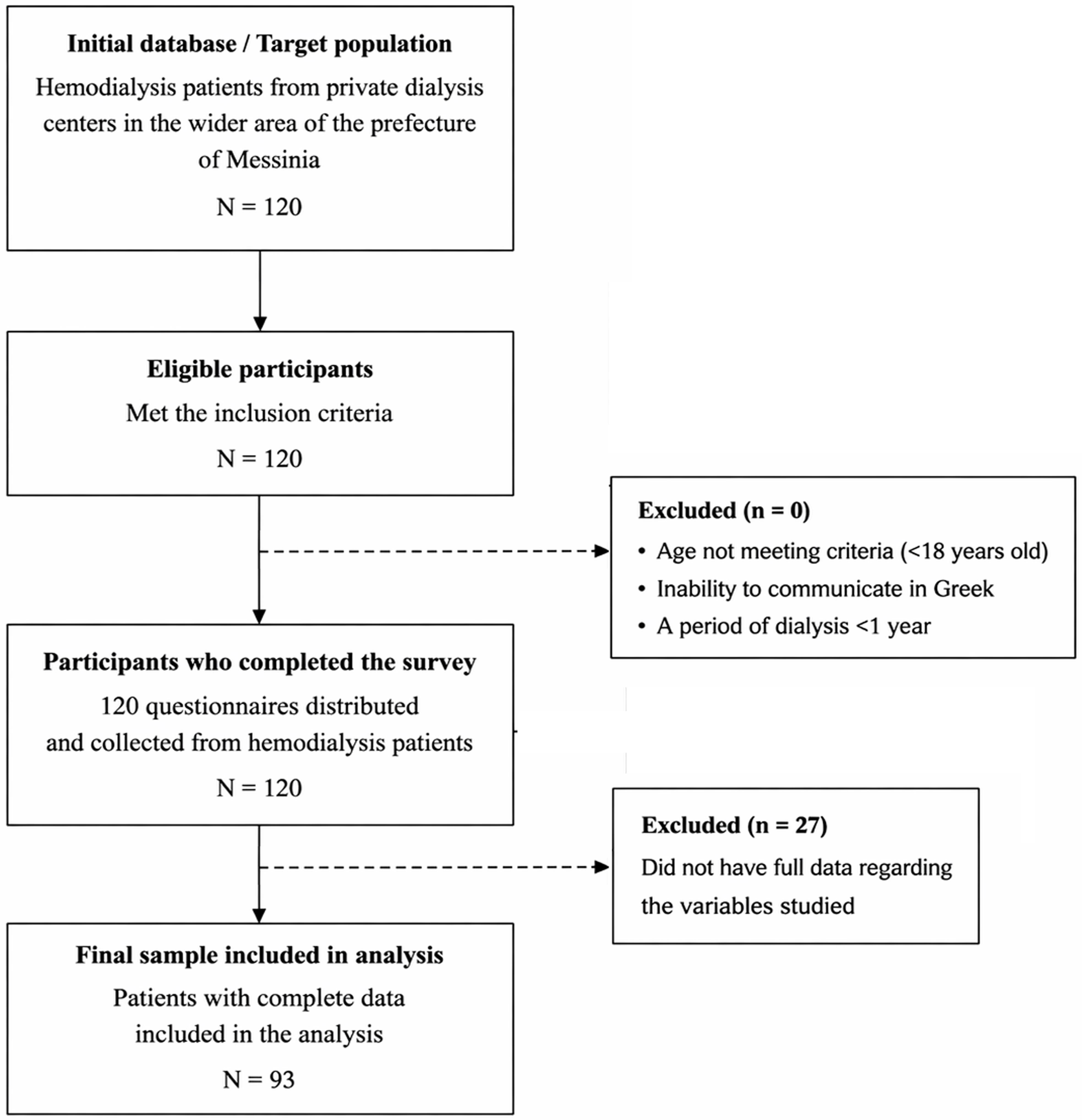
The method chosen for sample collection was convenience sampling. The sample that participated came from private dialysis centers in the wider area of the prefecture of Messinia. This study involved 120 patients with end-stage Chronic Renal Failure who underwent an extrarenal dialysis procedure, specifically hemodialysis. Of the 120 patients, 93 were selected and 27 were excluded, as they did not have full data regarding the variables studied (Fig. 1). The sample is adequate based on the fact that other similar studies were conducted including <100 renal patients.13 The inclusion criteria for the study included understanding the Greek language, a period of dialysis of at least one year, and age ranging from 30 to 95 years. The exclusion criteria were: <18 years old, inability to communicate in Greek, and a period of dialysis <1 year.
The following instruments were used to collect research data:
Missoula–VITAS Quality of Life Index-15 (MVQOLI-15): It is a psychometric self-report instrument with 5 basic dimensions. Its dimensions include: (1) the perception of physical discomfort and symptoms of the disease; (2) the perception of functionality and the performance of daily obligations or activities and the experiences of each individual in relation to personal expectations; (3) the levels of quality of life and interpersonal relationships; (4) the assessment of well-being; and finally (5) the presence or absence of spirituality. This questionnaire aims at the subjective and objective assessment of the actual situation and the percentage of influence of the present situation on the general quality of life.14
Self-Efficacy for Appropriate Medication Use Scale (SEAMS): The SEAMS questionnaire is a valid and reliable self-report instrument. It consists of thirteen items, with the lowest score being 13 and the highest being 39. A higher score indicates high levels of self-efficacy in taking medication. Each question has 3 answers, from which the patient can choose: not at all confident (score: 1), somewhat confident (score: 2), and very confident (score: 3). The purpose of this tool is to investigate the patient’s compliance rate in taking their medication at a specific point in time.15,16
Multidimensional Scale of Perceived Social Support (MSPSS): The MSPSS scale was created in 1988 and has been translated into many languages. In Greece, it was translated and adapted to cultural data by Theofilou. It aims to assess the perceived social support received by the patient. It is classified into 3 main categories, assessing the social support provided by family, friends, and social interactions with other categories. It consists of 12 questions, and its score ranges from 1 to 7 on a Likert scale, where 1 represents completely disagree and 7 represents completely agree. The total score ranges from 12 to 84, indicating low and high perceived social support, respectively.17 This questionnaire has successfully completed psychometric testing and is valid and reliable, easy to understand, and short.17
Spiritual Needs Questionnaire (SpNQ): The SpNQ questionnaire is a reliable and validated self-report tool and aims to assess the spiritual needs of the individual. It consists of 27 questions, which are classified into 4 categories of needs: the need for inner peace, the religious need, the need for contribution, and the existential need. Each question consists of 2 answers, which are scored with 1 if they agree and 0 if they disagree. If the answer indicating agreement is selected, then this answer is supplemented by a three-level Likert scale to indicate how strong this need is. These answers are scored from 1–3, where 1 indicates that this need is a little strong, 2 indicates the need is strong, and 3 indicates the need is very strong18
This research was approval by the Mesogeios ethics committees (approval number 123/7.5.2025). The Helsinki Declaration (as revised in 2024) was followed to involve human subjects in the study. Patients were informed about the nature of the research, its objectives, and the voluntary basis of their participation, ensuring their written consent in accordance with ethical standards and personal data protection principles. Questionnaires were self-administered.
The distributions of quantitative variables were tested for normality using the Kolmogorov–Smirnov test. For those that were normally distributed, the mean and standard deviations (SD) were used to describe them, while for those that were not normally distributed, the median and interquartile range were used. Absolute (N) and relative (%) frequencies were used to describe qualitative variables.
For the comparison between two quantitative variables, the Spearman correlation coefficient (rho) was used. Also, linear regression analysis was performed to investigate whether age, sex, education, and dialysis duration were predictive factors of quality of life and medication adherence. The significance levels were two-sided, and statistical significance was set at 0.05. The SPSS 26.0 statistical program was used for the analysis.
Results
The sample consisted of 93 participants with a mean age of 65.6 years (SD = 13.9 years), 62.4% of whom were male. 34.4% were elementary school graduates, 26.9% high school graduates, and 16.1% middle school graduates. The majority, 71%, were married. Also, almost half, 50.5%, were retired; 18.3% were housewives, while 10.8% were self-employed (Table 1).
Sociodemographic and clinical characteristics of the sample
| N | % | |
|---|---|---|
| Age, mean (SD), median (IQR) | 65.6 (13.9) | 68.0 (57–75) |
| Gender | ||
| Male | 58 | 62.4 |
| Female | 35 | 37.6 |
| Education | ||
| Municipal | 32 | 34.4 |
| Gymnasium | 15 | 16.1 |
| Lyceum | 25 | 26.9 |
| University | 12 | 12.9 |
| Postgraduate | 9 | 9.7 |
| Marital status | ||
| Single | 10 | 10.8 |
| Married | 66 | 71.0 |
| Divorced | 6 | 6.5 |
| Widowed | 11 | 11.8 |
| Professional employment | ||
| Unemployed | 7 | 7.5 |
| Private Employee | 7 | 7.5 |
| Civil servant | 5 | 5.4 |
| Freelancer | 10 | 10.8 |
| Housework | 17 | 18.3 |
| Pensioner | 47 | 50.5 |
| Student | 0 | 0.0 |
| Other | 0 | 0.0 |
| Years since diagnosis (kidney disease), mean (SD), median (IQR) | 11.5 (10.2) | 7.0 (5–16) |
| Have you undergone peritoneal dialysis? | ||
| No | 90 | 96.8 |
| Yes | 3 | 3.2 |
| Age of onset of hemodialysis | 60.5 (15.5) | 62.0 (54–72) |
| Chronic treatment (hemodialysis) | 5.2 (7.3) | 4.0 (2–6) |
| Has there been a transplant attempt in the past? | ||
| No | 83 | 89.2 |
| Yes | 10 | 10.8 |
| Have you expressed interest in participating in the transplant list? | ||
| No | 62 | 66.7 |
| Yes | 31 | 33.3 |
| If not, why? | ||
| Refusal | 35 | 56.5 |
| Fear | 12 | 19.4 |
| Insufficient information | 15 | 24.2 |
The median time since diagnosis of kidney disease was 7 years (interquartile range: 5–16 years), the median age at dialysis initiation was 62 years (interquartile range: 54–72 years), and the corresponding treatment time was 4 years (interquartile range: 2–6 years). Only 3.2% had undergone peritoneal dialysis, while 10.8% had attempted transplantation in the past. In addition, 33.3% had expressed interest in being on the transplant list. Among those who had not expressed interest, 56.5% did so due to refusal, 24.2% due to insufficient information, and 19.4% due to fear. Regarding interest in joining the transplant list, 66.7% of the patients answered “No”, while 33.3% answered “Yes” (Table 1).
The following table provides descriptive data for the dimensions and the total quality-of-life scale. Higher values for the dimensions and the total scale indicate better quality of life. The mean value for the symptom dimension was 8.9 points (SD = 7.8 points), for the functioning dimension was 5.9 points (SD = 7.9 points), for interpersonal relationships was 16.5 points (SD = 11.3 points), for well-being was −2.6 (SD=12.9 points), and for spirituality was 8.5 points (SD = 12.2 points). The mean total score for the quality-of-life scale was 18.9 points (SD = 3.2 points) (Table 2).
Descriptives of the questionnaires used
| Minimum value | Maximum value | Mean (SD) | Median (IQR) | |
|---|---|---|---|---|
| Symptoms | −16.0 | 30.0 | 8.9 (7.8) | 10 (5–12) |
| Functionality | −12.0 | 20.0 | 5.9 (7.9) | 8 (4–10) |
| Interpersonal relationships | −12.0 | 30.0 | 16.5 (11.3) | 16 (12–25) |
| Well-being | −25.0 | 30.0 | −2.6 (12.9) | −8 (−10–5) |
| Spirituality | −20.0 | 30.0 | 8.5 (12.2) | 9 (5–16) |
| Overall quality of life | 11.6 | 33.8 | 18.9 (3.2) | 18.7 (16.8–20.7) |
| Scale of self-efficacy for the appropriate use of medicines (SEAMS) | 16.0 | 48.0 | 40.1 (7) | 41 (36–46) |
| Spiritual needs scale (SpNQ) | 0.0 | 2.9 | 1.1 (0.7) | 0.9 (0.5–1.7) |
| MSPSS | ||||
| Total support | 1.0 | 7.0 | 5.8 (1.1) | 5.9 (5–6.7) |
| Family support | 1.0 | 7.0 | 6.2 (1) | 6.8 (5.6–7) |
| Support from friends | 1.0 | 7.0 | 5 (1.5) | 5 (4–6) |
| Partner support | 1.0 | 7.0 | 6.1 (1.1) | 6.8 (5.3–7) |
Accordingly, descriptive data are given for the self-efficacy scale in taking medication, which can range from 16 to 48 units, and higher values correspond to greater self-efficacy. In this specific sample, the mean value on this scale was 40.1 units (SD = 7) (Table 2).
The scale of SpNQ is the average of its questions and can range from 0 to 3 points, with higher values corresponding to increased spiritual needs. In this sample, it ranged from 0 to 2.9 points, with a mean value of 1.1 points (SD = 0.7) (Table 2).
Regarding social support dimensions, all range from 1 to 7 points, and higher values indicate greater support. The support dimension from family had a mean value of 6.2 points (SD = 1 point), from friends had a mean value of 5 points (SD = 1.5 points), and from a partner had a mean value of 6.1 points (SD = 1.1 points). The total support had a mean value of 5.8 points (SD = 1.1 points) (Table 2).
The following are the Spearman correlation coefficients for the quality of life, self-efficacy for appropriate medication use, spiritual needs, and social support scales. Greater self-efficacy was associated with better interpersonal relationships, greater spirituality, and generally better quality of life. Correspondingly, increased spiritual needs were associated with better interpersonal relationships and overall better quality of life. Stronger social support was associated with better interpersonal relationships, greater spirituality, and generally better quality of life. It was also associated with greater self-efficacy regarding medication intake. Greater support from family and friends was associated with better interpersonal relationships, overall better quality of life, and greater self-efficacy regarding medication intake. Support from a partner was also significantly associated with better quality of life regarding symptoms, better interpersonal relationships, greater spirituality, generally better quality of life, and greater self-efficacy regarding medication intake. There was also a significant correlation between the spiritual needs scale and dimensions of support from family and partner. Greater support from them was associated with increased spiritual needs (Table 3).
Correlation among variables
| Scale of self-efficacy for the appropriate use of medicines | Spiritual needs scale | Total support | Family support | Support from friends | Partner support | |
|---|---|---|---|---|---|---|
| Symptoms | ||||||
| rho | 0.07 | 0.01 | 0.07 | 0.16 | −0.07 | 0.25 |
| P | 0.495 | 0.909 | 0.480 | 0.124 | 0.514 | 0.016 |
| Functionality | ||||||
| rho | −0.01 | −0.11 | 0.01 | 0.13 | 0.03 | 0.04 |
| P | 0.981 | 0.299 | 0.917 | 0.204 | 0.787 | 0.742 |
| Interpersonal relationships | ||||||
| rho | 0.41 | 0.33 | 0.47 | 0.52 | 0.36 | 0.38 |
| P | <0.001 | 0.001 | <0.001 | <0.001 | <0.001 | <0.001 |
| Well-being | ||||||
| rho | 0.12 | 0.14 | 0.06 | −0.02 | 0.11 | 0.08 |
| P | 0.247 | 0.188 | 0.549 | 0.876 | 0.283 | 0.424 |
| Spirituality | ||||||
| rho | 0.25 | 0.11 | 0.24 | 0.14 | 0.19 | 0.29 |
| P | 0.016 | 0.317 | 0.023 | 0.200 | 0.075 | 0.004 |
| Overall quality of life | ||||||
| rho | 0.29 | 0.20 | 0.30 | 0.25 | 0.27 | 0.35 |
| P | 0.004 | 0.050 | 0.004 | 0.015 | 0.010 | 0.001 |
| Scale of self-efficacy for the appropriate use of medicines | ||||||
| rho | 1.000 | −0.12 | 0.40 | 0.23 | 0.44 | 0.24 |
| P | 0.256 | <0.001 | 0.028 | <0.001 | 0.019 | |
| Spiritual needs scale | ||||||
| rho | 0.20 | 0.37 | 0.05 | 0.27 | ||
| P | 0.062 | <0.001 | 0.637 | 0.009 |
By examining the association of quality of life with years since diagnosis, age on dialysis, and years of treatment, it was found that older age was associated with better functionality, while, conversely, more years in treatment were associated with worse quality of life in terms of symptoms (Table 4).
Correlation of clinical characteristics to quality of life
| Years since diagnosis (kidney disease) | Age of starting dialysis | Chronic treatment (hemodialysis) | |
|---|---|---|---|
| Symptoms | |||
| rho | −0.17 | 0.05 | −0.23 |
| P | 0.101 | 0.649 | 0.024 |
| Functionality | |||
| rho | −0.18 | 0.21 | −0.06 |
| P | 0.085 | 0.048 | 0.553 |
| Interpersonal relationships | |||
| rho | 0.05 | −0.07 | 0.02 |
| P | 0.632 | 0.518 | 0.854 |
| Well-being | |||
| rho | 0.12 | −0.15 | 0.05 |
| P | 0.237 | 0.153 | 0.618 |
| Spirituality | |||
| rho | 0.05 | −0.14 | −0.01 |
| P | 0.619 | 0.196 | 0.933 |
| Overall quality of life | |||
| rho | −0.01 | −0.08 | −0.11 |
| P | 0.919 | 0.472 | 0.299 |
Age at dialysis initiation was found to be associated with medication self-efficacy. Older age at dialysis initiation was associated with decreased self-efficacy (Table 5).
Association of clinical characteristics with medication adherence
| Years since diagnosis | Age of starting dialysis | Chronic treatment (hemodialysis) | |
|---|---|---|---|
| Scale of self-efficacy for the appropriate use of medicines | |||
| rho | 0.08 | −0.24 | 0.04 |
| P | 0.463 | 0.018 | 0.707 |
Regarding linear regression analysis, statistically significant results were observed in the dependent variable of functionality, with age being a predictor (P = 0.013, Beta = 0.285), as well as in well-being, with education being a predictor (P = 0.046, Beta = 0.231).
Discussion
The research conducted investigated the effect of various dimensions of social support and spirituality on the quality of life and compliance with medication in patients undergoing hemodialysis. The sample analyzed comes from 93 patients with an average age of 65.5 years and an average time on hemodialysis of 4 years. The majority of them are men (62.4%), and the educational level varies. Equally important to mention is the high percentage of married people—who constitute 71% of the sample—as well as the percentage of interest in transplantation, which is lower than expected (33.3%). The inclusion criteria required that participants had been undergoing hemodialysis for at least one year, allowing sufficient time for adaptation to the treatment and adjustment to changes in their daily lives. Also, there was an age restriction of 18 to 95 years, while understanding the Greek language was necessary, as the questionnaires were in Greek and initially required understanding and, by extension, completion.
The results derived from the analysis of the scores of the tools used are in agreement with numerous studies that have been carried out in this field. More specifically, in the MVQOL quality-of-life scale, the results of each dimension ranged around the average values of the questionnaire, presenting a moderate to poor quality of life for the respondents. This result complements that of previous studies—as well as the common understanding from which this research was inspired—that the quality of life of patients undergoing hemodialysis is low and needs immediate investigation to find factors that can improve it.19 On the contrary, in the SEAMS medication self-efficacy scale, the result was quite encouraging, since the average score of the participants was 40.1, almost at the upper limit of the scale, presenting a very good dimension of patients’ understanding and compliance with the instructions of health professionals.
The correlation of high self-efficacy with general compliance with medication has been studied and confirmed by other studies, such as that of Náfrádi et al.20 Correspondingly high values were observed in the social support scale, where the averages of the respondents were very close to the upper limit of the scale for all its dimensions, which shows that the social support perceived by the patients is very high. This result is very encouraging and becomes particularly interesting when the correlation of social support with the improvement of quality of life and compliance with medication is also observed. More specifically, the correlation among the scales reveals a positive connection of the dimensions of perceived social support with increased levels of quality of life, increased self-efficacy in compliance with medication, as well as increased levels of spirituality. This result is in agreement with numerous studies that have shown the significant relation of social support to the lives of patients with CKD.1,4,5
Regarding the SpNQ spiritual needs questionnaire, the average score of the respondents was below average, revealing the low level of spirituality of the patients. However, there seems to be a positive association of spirituality with both the quality of life of patients and their interpersonal relationships. Similar conclusions have been drawn from other studies, such as that of Davison & Jhangri.9 Nevertheless, its correlation with multiple parameters makes it an interesting point for investigation. From the above data that were collected and analyzed, it can be concluded that investigating the lives of hemodialysis patients can be significantly correlated to both their health status and their quality of life. To achieve this goal, however, further investigation and a holistic approach to these patients, as well as the difficulties they face, are required.
Concerning the study limitations, the sample is small and may not reveal significant correlations in the data. It would be interesting to conduct more relevant studies in Greece using more variables and evaluating more dimensions in the context of multiple comparisons (multivariable analysis adjusting for confounding factors like age, gender, education, or dialysis duration). It would also be beneficial to obtain data from a larger number of patients, which would allow for the identification of more significant associations and the generalizability of the results. Selection bias caused by convenience sampling, as well as the inability of the cross-sectional design to establish causal relationships, are some weaknesses of the present study.
Conclusions
The findings of the present study could be used in the development of health care services as well as in patient management. Spiritual beliefs, in particular, may play an important role in the course of illness and treatment outcomes and could therefore be identified as an area for psychological intervention in individuals with end-stage renal disease. Further, interventions are suitable for those patients with low social support.
Declarations
Acknowledgement
The authors would like to thank the patients for their participation in the present study.
Ethical statement
This research was approval by the Mesogeios ethics committees (approval number 123/7.5.2025). The Helsinki Declaration (as revised in 2024) was followed to involve human subjects in the study. Patients were informed about the nature of the research, its objectives, and the voluntary basis of their participation, ensuring their written consent in accordance with ethical standards and personal data protection principles. Questionnaires were self-administered.
Data sharing statement
Data related to this research can be found within this article.
Funding
None.
Conflict of interest
The authors declare no conflict of interest.
Authors’ contributions
Conception and design, supervision, visualization, manuscript review, and editing (PT, MB), data collection, analysis, drafting of the original manuscript (PT, MB), drafting and critical revision of the manuscript (PT, MB), drafting of the original manuscript and figure preparation (PT, MB), supervision, visualization, manuscript writing, review, and editing (PT, MB). All authors have approved the final version and publication of the manuscript.

 Author information
Author information